
Chiropractor Chandler AZ
PLATELET-RICH PLASMA PROLOTHERAPY FOR IT BAND TENDONITIS

IT band stands for the Iliotibial Band which is a band of thick connective tissues that runs along the sides of the hip. The most important role of the IT band is in the movement of the thigh as it connects hip muscles to the tibia of the lower leg. The IT band starts at the iliac crest in the pelvis, tracks down along the outer thigh, crosses the knee joint and connects with the top part of the tibia bone. It is a deep fascia of the body and, like other deep fascia of the body, it is made of regular, thick connective tissues that are very strong and avascular.
In the IT band, the collagen fibres are arranged in straight lines that give them strength. A small number of elastin proteins are also present in the IT band which gives some elasticity to the band. The function of the IT band is to provide stability to the hip and the knee and prevent dislocation of these joints. The IT band can overdevelop and rub against the hip bone or the outer knee every time the knee is bent or the hip is flexed. It is more common in athletes and cyclists. It can lead to IT band tendonitis that is also called IT band syndrome. IT band tendonitis is the most common cause of running injuries. It comprises 12% of all running-related injuries.
CAUSES OF IT BAND TENDONITIS
IT band tendonitis is caused by overuse of the IT band and it occurs in long distant runners, cyclists, and other athletes. It can be caused by a combination of causes such as:
- Poor training habits
- Poor muscle flexibility
- Mechanical imbalance in the body especially in lower back, pelvis, hips, and knees
- Heavy weight lifting
Some of the risk factors of IT band tendonitis are following:
- Leg length discrepancy
- Abnormal tilt to the pelvis
- Bowed legs
- Pain in the lateral side of the knee is the most common sign and it is due to the inflammation of the IT band
- Stinging sensation in the knee
- Popping sound at the knee
- Pain in the hip area
- Swelling around the knee where the IT band joins the tibia
- Pain that improves with rest
- Tenderness
DIAGNOSIS OF IT BAND TENDONITIS
PHYSICAL EXAMINATIONThe doctor will observe the patient's knee area. Patients suffering from IT band tendonitis will have tenderness 2 cm above the knee and the tenderness will worsen when the patient is in a standing position. The doctor can also perform Ober's test to evaluate the tightness of the IT band.
IMAGING TECHNIQUESThe clinical diagnosis of the IT band is mostly based on the history of the patient and physical examination, but if any other reason of pain is suspected, the doctor can recommend an MRI to get a detailed image of the pelvis, hip, and knee area. In patients with IT band tendonitis, the MRI results show a thickened IT band over lateral femoral epicondyle and fluid retention in the IT band. An X-ray is not recommended for IT band tendonitis.
TREATMENT OF IT BAND TENDONITIS
CONVENTIONAL/ NON-SURGICAL TREATMENTThe initial treatment of IT band tendonitis is ice, rest and compression, and elevation. In most of the cases, the situation is improved by taking proper rest.
Home treatments can include massage, stretching, and the use of roller foam at the site of pain and swelling.
To relieve the pain, non-inflammatory medications such as ibuprofen (Advil, Motrin) and naproxen (Aleve) can be prescribed.
If these initial treatment options fail to relieve the pain, the next step is physical therapy. The physical therapist can help the patient to strengthen the IT band and reduce the swelling. Physical therapy also improves the muscle strength, flexibility, and the stability that is helpful in treating IT band tendonitis.
Therapeutic ultrasound can also be used to treat IT band tendonitis. It can be phonophoresis in which the anti-inflammatory medicine is pushed through the skin to the inflamed part or iontophoresis in which electricity is used instead of ultrasound.
If the medication and physical therapy fail to relieve the pain, corticosteroids such as dexamethasone, methylprednisolone, and hydrocortisone are injected at the site of pain and inflammation. Corticosteroid injections are a short term solution and excessive use can damage and weaken the IT band.
SURGICAL TREATMENTIn most of the IT band tendonitis cases, the conventional treatment options are helpful in relieving the pain and inflammation, but in some cases, these methods fail to improve the situation. Therefore, in such cases, surgery is the only option left. Arthroscopy is used to locate the inflammation around the IT band and cut it away. Another surgical option is to cut a triangular shape portion of the IT band to increase the IT band length and provide more space for it to slide across bone.
ALTERNATIVE TREATMENT OPTIONSome people suffering from IT band tendonitis fail to respond to conventional treatment options and they have to stop participating in athletic activities to prevent any further damage to the IT band. In the past few years, a new treatment option known as Platelet-rich plasma (PRP) Prolotherapy is being introduced as an effective treatment option for non-responsive IT band tendonitis. PRP Prolotherapy is a part of a new branch of medicine known as Regenerative Medicine. It uses the body's healing ability to repair the damage and relieve the pain and inflammation. The platelet-rich plasma Prolotherapy works on a very simple principle: "when the platelet concentration is increased in a certain area of the body, it accelerates the healing process." Platelets contain many chemicals known as:
- Glycogen
- Lysosomes
- Alpha granules
- Beta granules
Alpha granules contain growth factors and they are the main focus of platelet-rich plasma therapy. There are three stages of healing after platelet-rich plasma Prolotherapy injection and different types of growth factors are involved in driving different stages.
- Inflammation phase: It lasts for 2-3 days. In this phase, growth factors are released.
- Proliferation phase: It lasts for 2-4 weeks. It is vital for musculoskeletal regeneration.
- Remodelling phase: It lasts over a year. In this phase, collagen is matured and strengthened and the injury is healed.
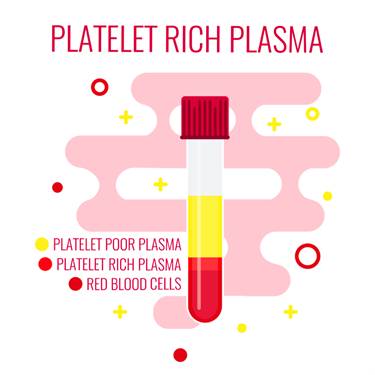
20-30 mL of blood is used to make platelet-rich plasma. The blood is spun for 15 minutes at 3,200 rpm in a centrifuge machine. This step separates platelet-rich plasma from platelet-poor plasma. 3 mL of platelet-rich plasma is obtained from 20 mL of blood. The platelet-rich plasma is combined with half mL of sodium bicarbonate to neutralise its pH. The injection is administered with the help of dynamic musculoskeletal ultrasound with a transducer of 6–13 Hz to maximise the location accuracy for the injection. The injection is administered directly at the site of injury.
As the platelet-rich plasma Prolotherapy technique uses the patient's own blood, the chances of immunogenic reaction or the transfer of blood borne diseases are completely eliminated.
The growth factors attach to the cell surface and not the nucleus of the cell; thus the chances of tumour growth are also eliminated. As the platelet-rich plasma Prolotherapy is an injection-based procedure, the risks involved in the procedure are:
- Anaesthesia allergy
- Infection
- Neural trauma
- Organ trauma
- Needle breakage
PRP prolotherapy is an effective option for the treatment of IT band tendonitis. Research data is available which shows that PRP prolotherapy is an effective and safe treatment option for IT band tendonitis. The most recent research in Regenerative Medicine shows that PRP prolotherapy has great anti-inflammatory properties as it inhibits Cox-1 and Cox-2 proteins in the inflammatory pathway that leads to pain reduction and increased recovery with minimum to no side effect.
In 2012, in a meta-analysis, the efficiency of steroid injection and PRP Prolotherapy were compared. The results showed that the effect of steroid injections was very short term as compared to PRP injections, but PRP needs more research to determine the duration of efficiency.
When a study was conducted on the patients with chronic elbow tendonitis, the group that received PRP injections showed a 60% decrease in pain as compared to the control group which showed only a 16% decrease. There are high chances that PRP prolotherapy will be as helpful in treating IT band tendonitis as it is in treating elbow tendonitis. A combination of PRP Prolotherapy and Physical therapy is more effective to treat hip pain as compared to Physical therapy alone.
According to a research study published in May 2015, doctors articulated concerns over the lack of standardization of PRP Prolotherapy. Research done in the past 10 years acknowledged that the role of PRP in bone, tendon, cartilage, and ligament tissue regeneration is very promising, but some controversial results have also arisen.
CONSERVATIVE TREATMENTS TO COMBINE WITH PRPWhile PRP and stem cell treatments are enhancing the tissue repair and regeneration, conservative treatments can enhance healing, strengthen the muscles, and stabilize joint movements to maximize your recovery.
COLD LASER THERAPY TREATMENTS:
- Accelerated tissue repair and cell growth
- Faster wound healing
- Reduced fibrous tissue formation
- Anti-inflammation
- Pain relief
- Increased blood flow
- Increased repair and regeneration
- Nerve function and repair
- Increased energy production- ATP
Photons of light from lasers penetrate into tissue and accelerate cellular growth and reproduction. Laser therapy increases the energy available to the cell so it can work faster, better, and quickly get rid of waste products. When cells of tendons, ligaments, and muscles are exposed to laser light they repair and heal faster.

Laser light increases collagen production by stimulating fibroblasts. Collagen is the building block of tissue repair and healing. Laser therapy increases fibroblast activity and therefore collagen production to speed healing.
Low-level laser therapy decreases scar tissue formation. Scar tissue can be a source of chronic pain and poor healing. By eliminating excessive scar tissue and encouraging proper collagen production, painful scars and chronic pain is reduced.
Laser therapy causes vasodilatation (increases the size of capillaries) which increases blood flow. The treatments also increases lymphatic drainage to decrease swelling or edema. Therefore, laser therapy reduces swelling caused by bruising or inflammation while speeding the recovery process.
Cold laser therapy decreases pain by blocking pain signals to the brain. Some nerve cells sense pain and send signals to the brain. Chronic pain can be caused by overly active pain nerves. Specific wavelengths help "shut off" the pain signals, thereby eliminating your pain.
Low-level lasers are excellent at decreasing inflammation, which also increases pain nerve activity. Cold laser therapy also increases endorphins and enkephalins, which block pain signals and decrease pain sensation. Overall laser therapy reduces painful nerve signals and reduces your perceived pain.
Blood carries nutrients and building blocks to the tissue, and carries waste products away. Increased blood flow to tissues increases and enhances cellular healing. Cold laser therapy increases the formation of capillaries in damaged tissue. Specific laser frequency also increases blood flow to the area treated to enhance injury repair.
Low-level lasers increases enzyme activity to improve metabolic activity that affects cell repair and regeneration. The enzymes are turned on "high" to speed the healing.
Nerves heal very slowly. Lasers speed up this process. Damage to nerves causes numbness, pain, muscle weakness, and altered sensations. Laser therapy treatments enhance nerve function, healing, and reduce pain.
ATP is like gasoline for cells, it is the energy source that cells operate. Injured cells often have low levels of ATP, which decreases their ability to heal and repair. By increasing ATP and "gasoline storage levels," cells have the ability to heal and repair.
Therapeutic treatments for addressing soft tissue injuries involve massage therapy, manual therapy, trigger point therapy, Graston Technique, or Active Release Technique. These treatments increase blood flow, decrease muscle spasms, enhance flexibility, speed healing, and promote proper tissue repair.
When these treatments are incorporated into a treatment plan, patients heal faster and are less likely to have long-term pain, soft tissue fibrosis, or scar tissue in the injured muscle. These soft tissue treatments are incorporated with therapeutic exercises and flexibility programs.

Many leg injuries are associated with radiating pain. The two legs function as a system for movement. Injuries in one area of the system are commonly associated with poor joint stabilization in the foot, knee, or hip. This leads to poor alignment and excessive forces being placed onto muscles and tendons. Knee injuries are common because of weakness and poor stabilization of the leg and hip muscles. The combination of muscle weakness, poor coordination, and altered gait mechanics produce excessive strain on the soft tissues.
The lower extremities work as a comprehensive unit performing many of the repetitive tasks at home, work, and recreational sports. Injuries to one area of the musculature often indicate that additional damage has been incurred by other muscles.

Many therapeutic exercises can help restore proper strength and endurance to the leg muscles. Isometric exercises are often the initial treatment exercises, followed by single plane rubber band exercises for hip, knee, and ankle; flexion, extension, adduction, abduction, circumduction, inversion, and eversion. Dynamic exercises involving stability foam, rubber discs, exercise balls, and BOSU balls can be performed on the floor. The more unstable of the surface the more effort and stabilization is required of all the lower extremity muscles.
Vibration plates enhance neuromuscular learning throughout the ankle, knee, foot, hip, and back muscles. Additional strength exercises can be found on the hip, knee, and foot strengthening pages. More information for injuries and treatments foot pain and exercises.
BIBLIOGRAPHY:
Adere, J., & Louw, Q. A. (2015). Biomechanical risk factors associated with iliotibial band syndrome in runners: a systematic review. BMC Musculoskelet Disord.
Baker, R. L., & Fredericson, M. (2016). Iliotibial Band Syndrome in Runners: Biomechanical Implications and Exercise Interventions. Phys Med Rehabil Clin N Am, 53-77.
English, S., & Perret, D.(2010). Posterior knee pain. Curr Rev Musculoskelet Med, 3-10.