
Chiropractor Chandler AZ
PLATELET-RICH PLASMA PROLOTHERAPY FOR HIP BURSITIS
Bursae (Singular: Bursa) are small sacs that have a jelly-like structure and are found throughout the human body including the shoulder, elbow, hip, knee, and heel. Bursae contain fluids and are found between bones and soft tissues where they act as a cushion to reduce friction during movement.
Bursitis is swelling of the bursa. In the hip joint, there are two main bursae that are swelled and cause pain. Trochanteric bursitis is the swelling of the bursa that is present on the great trochanter of the femur bone. Another type is iliopsoas bursa that is found on the inner side of the hip. When iliopsoas bursa is swollen, it is also called hip bursitis. The pain in this condition is located in the groin area. This condition is less common than trochanteric bursitis, but treatment for both conditions is the same.

SYMPTOMS OF HIP BURSITIS
The main symptom of the trochanteric bursitis is a pain in the hip joint. This pain spreads towards the outer side of the hip joint. This pain is sharp and intense during the early stages of bursitis. During the advanced stages, the pain may become more of an ache and can cover the larger hip joint area.
The pain caused by hip bursitis can get worse at night, especially after lying on the affected hip joint. It can also get worse when the patient stands up from a chair after sitting for a long period of time. Prolonged walking, climbing stairs or squatting can also make it get worse.
RISK FACTORS OF HIP BURSITISHip bursitis can affect anyone, but women and elderly people are more affected than others. It is less common in men and young people. There are certain risk factors associated with the development of hip bursitis such as:
REPETITIVE STRESS
Repetitive stress or overuse of the hip joint such as running, climbing stairs, bicycling and standing for long periods of time can lead to inflammation of the hip bursa.
HIP INJURYA hip injury can be due to falling onto the hip or lying on one side of the body for a long duration and it can lead to hip bursitis.
SPINE DISEASESSpine diseases like scoliosis and arthritis can lead to hip bursitis.
UNEQUAL LEG LENGTHThe hip bursa can be affected in a case where one leg is significantly shorter than the other. This condition affects the walk of the person which can put stress on the hip bursa and can lead to bursitis.
RHEUMATOID ARTHRITISRheumatoid arthritis can also lead to swelling of the hip bursae.
PREVIOUS SURGERYThe hip bursa can be irritated by hip surgery or a prosthetic implant in the hip and it can lead to bursitis.
BONE SPURSBone spurs, also known as calcium deposits, can develop within the tendons of the trochanter. These deposits can irritate the bursa and can lead to bursitis.

DIAGNOSIS OF HIP BURSITIS
PHYSICAL EXAMINATIONThe doctor will perform a comprehensive physical examination of the hip joint to diagnose hip bursitis. Tenderness in the hip area is a sign of hip bursitis.
TESTSThe doctor can order different tests to confirm the diagnosis. These tests can be:
X-ray: A simple X-ray can show the swollen bursa in the hip joint, confirming the diagnosis of hip bursitis.
Magnetic resonance imaging (MRI): Detailed images of the hip is obtained by MRI which helps in diagnosing any underlying causes of hip pain.
Computer tomography (CT scan): A CT scanner takes several X-rays and a detailed image of the hip joint is developed by a computer which gives an even more detailed picture to diagnose minor injuries as well.
TREATMENT OF HIP BURSITIS
NONSURGICAL TREATMENTThe initial treatment of hip bursitis is lifestyle changes that can help to relieve the pain caused by hip bursitis. These changes include:
Activity changes: It involves avoiding the activities that can increase the pain. Opting for less intense activities instead of high-intensity activities is recommended.
Non-steroidal anti-inflammatory drugs (NSAIDs): drugs like ibuprofen, naproxen and piroxicam can be helpful in relieving the pain caused by a swollen bursa. But NSAIDs can only be taken for a short period of time and the patient must consult the doctor before taking these drugs as they can cause serious side effects in patients with certain medical conditions.
Assistive devices: Hip bursitis patients are recommended to use assistive devices such as a walking cane or crutches for a week or more to remove pressure from the hip joint and relieve the pain.
Physical therapy: exercises that increase hip strength and flexibility are helpful in relieving hip bursitis pain. The patient can do the exercises on his own or a physical therapist can teach him how to do the exercise. Physical therapy also uses other treatments such as massage therapy, ice, and heat.
Steroid injection: if the other options fail to relieve the pain, corticosteroid injections are suggested along with local anesthesia. This is a simple and effective treatment in which a corticosteroid is injected into the hip bursa. A corticosteroid injection can provide temporary or permanent relief, but long term use of these injections can damage the surrounding tissues and increase the damage in the hip joint.
SURGICAL TREATMENTSurgery is not a common option in the case of hip bursitis. If the nonsurgical treatment options fail to reduce the swelling and pain, then the doctors can recommend surgical removal of the bursa. Removal of bursa does not affect the hip functionality.
Arthroscopic removal of the bursa is the advanced technique in which the bursa is removed through a small cut over the hip. Arthroscopy is a small camera that is inserted into the hip through another incision so that the doctor can see the inside of the joint. It is a less invasive surgery and recovery time is minimum.
ALTERNATIVE TREATMENT OPTIONHip bursitis is a painful condition and it can lead to impairment of daily activities. The treatment approach of hip bursitis is based on pain management and it is less focused on treating the actual cause of bursitis which is inflammation. A treatment option that treats the cause of the hip bursitis will be helpful in relieving the pain and protecting the structure of the hip joint. Some work is being done on this approach and Platelet-rich plasma prolotherapy is being used to treat such problems with the help of the body's own repair machinery. PRP prolotherapy is a part of a new branch of medicine known as Regenerative Medicine. It uses the body's healing ability to repair the damage and relieve the pain and inflammation. The platelet-rich plasma Prolotherapy works on a very simple principle: "when the platelet concentration is increased in a certain area of the body, it accelerates the healing process." Platelets contain many chemicals known as:
- Glycogen
- Lysosomes
- Alpha granules
- Beta granules
Alpha granules contain growth factors and they are the main focus of platelet-rich plasma therapy. There are three stages of healing after platelet-rich plasma Prolotherapy injections and different types of growth factors are involved in driving different stages:
- Inflammation phase: It lasts for 2-3 days. n this phase, growth factors are released.
- Proliferation phase: It lasts for 2-4 weeks. It is vital for musculoskeletal regeneration.
- Remodeling phase: It lasts over a year. In this phase, collagen is matured and strengthened and injury is healed.
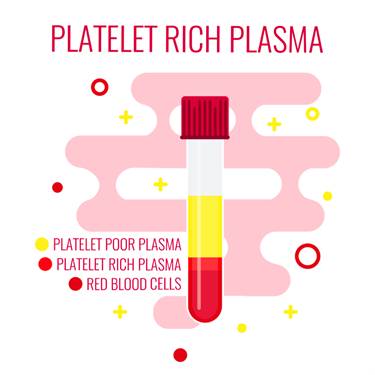
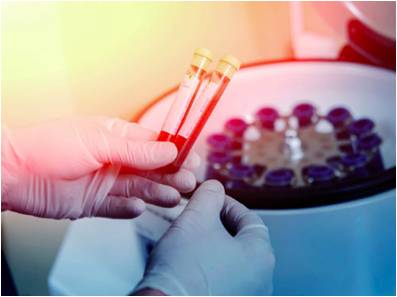
20-30 mL of blood is used to make platelet-rich plasma. The blood is spun for 15 minutes at 3,200 rpm in a centrifuge machine. This step separates platelet-rich plasma from platelet-poor plasma. 3 mL of platelet-rich plasma is obtained from 20 mL of blood. The platelet-rich plasma is combined with half mL of sodium bicarbonate to neutralize its pH. The injection is administered with the help of a dynamic musculoskeletal ultrasound with a transducer of 6–13 Hz to maximize the location accuracy for the injection. The injection is administered directly at the site of injury.
As platelet-rich plasma Prolotherapy technique uses the patient's own blood, the chances of immunogenic reaction or the transfer of blood borne diseases are completely eliminated.
The growth factors attach to the cell surface and not the nucleus of the cell, thus the chances of tumor growth are also eliminated. As the platelet-rich plasma Prolotherapy is an injection-based procedure, the risks involved in the procedure are:
- Anaesthesia allergy
- Infection
- Neural trauma
- Organ trauma
- Needle breakage
There are several research results available that show that effectiveness of PRP in reducing inflammation. The most recent research in Regenerative medicine shows that PRP prolotherapy has great anti-inflammatory properties as it inhibits Cox-1 and Cox-2 proteins in the inflammatory pathway that leads to pain reduction and increased recovery with minimum to no side effects.
According to a new research, PRP prolotherapy is more effective than steroid injections in case of hip bursitis.
In a research study published in May 2015, doctors expressed concerns over the lack of standardization of PRP Prolotherapy. Research done in the past 10 years acknowledged that the role of PRP in bone, tendon, cartilage, and ligament tissue regeneration is very promising, but some controversial results have also arisen.
CONSERVATIVE TREATMENTS TO COMBINE WITH PRP
While PRP and stem cell treatments are enhancing the tissue repair and regeneration, conservative treatments can enhance healing, strengthen the muscles, and stabilize joint movements to maximize your recovery.
COLD LASER THERAPY TREATMENTS
- Accelerated tissue repair and cell growth
- Faster wound healing
- Reduced fibrous tissue formation
- Anti-inflammation
- Pain relief
- Increased blood flow
- Increased repair and regeneration
- Nerve function and repair
- Increased energy production- ATP

Photons of light from lasers penetrate into tissue and accelerate cellular growth and reproduction. Laser therapy increases the energy available to the cell so it can work faster, better, and quickly get rid of waste products. When cells of tendons, ligaments, and muscles are exposed to laser light they repair and heal faster.
Laser light increases collagen production by stimulating fibroblasts. Collagen is the building block of tissue repair and healing. Laser therapy increases fibroblast activity and therefore collagen production to speed healing.
Low-level laser therapy decreases scar tissue formation. Scar tissue can be a source of chronic pain and poor healing. By eliminating excessive scar tissue and encouraging proper collagen production, painful scars and chronic pain is reduced.
Laser therapy causes vasodilatation (increases the size of capillaries) which increases blood flow. The treatments also increases lymphatic drainage to decrease swelling or edema. Therefore, laser therapy reduces swelling caused by bruising or inflammation while speeding the recovery process.
Cold laser therapy decreases pain by blocking pain signals to the brain. Some nerve cells sense pain and send signals to the brain. Chronic pain can be caused by overly active pain nerves. Specific wavelengths help "shut off" the pain signals, thereby eliminating your pain.
Low-level lasers are excellent at decreasing inflammation, which also increases pain nerve activity. Cold laser therapy also increases endorphins and enkephalins, which block pain signals and decrease pain sensation. Overall laser therapy reduces painful nerve signals and reduces your perceived pain.
Blood carries nutrients and building blocks to the tissue, and carries waste products away. Increased blood flow to tissues increases and enhances cellular healing. Cold laser therapy increases the formation of capillaries in damaged tissue. Specific laser frequency also increases blood flow to the area treated to enhance injury repair.
Low-level lasers increases enzyme activity to improve metabolic activity that affects cell repair and regeneration. The enzymes are turned on "high" to speed the healin
Nerves heal very slowly. Lasers speed up this process. Damage to nerves causes numbness, pain, muscle weakness, and altered sensations. Laser therapy treatments enhance nerve function, healing, and reduce pain
ATP is like gasoline for cells, it is the energy source that cells operate. Injured cells often have low levels of ATP, which decreases their ability to heal and repair. By increasing ATP and "gasoline storage levels," cells have the ability to heal and repair
SOFT TISSUE TREATMENTS
Therapeutic treatments for addressing soft tissue injuries involve massage therapy, manual therapy, trigger point therapy, Graston Technique, or Active Release Technique. These treatments increase blood flow, decrease muscle spasms, enhance flexibility, speed healing, and promote proper tissue repair.
When these treatments are incorporated into a treatment plan, patients heal faster and are less likely to have long-term pain, soft tissue fibrosis, or scar tissue in the injured muscle. These soft tissue treatments are incorporated with therapeutic exercises and flexibility programs.

Many leg injuries are associated with radiating pain. The two legs function as a system for movement. Injuries in one area of the system are commonly associated with poor joint stabilization in the foot, knee, or hip. This leads to poor alignment and excessive forces being placed onto muscles and tendons. Knee injuries are common because of weakness and poor stabilization of the leg and hip muscles. The combination of muscle weakness, poor coordination, and altered gait mechanics produce excessive strain on the soft tissues.
The lower extremities work as a comprehensive unit performing many of the repetitive tasks at home, work, and recreational sports. Injuries to one area of the musculature often indicate that additional damage has been incurred by other muscles.

Many therapeutic exercises can help restore proper strength and endurance to the leg muscles. Isometric exercises are often the initial treatment exercises, followed by single plane rubber band exercises for hip, knee, and ankle; flexion, extension, adduction, abduction, circumduction, inversion, and eversion. Dynamic exercises involving stability foam, rubber discs, exercise balls, and BOSU balls can be performed on the floor. The more unstable of the surface the more effort and stabilization is required of all the lower extremity muscles.
Vibration plates enhance neuromuscular learning throughout the ankle, knee, foot, hip, and back muscles. Additional strength exercises can be found on the hip, knee, and foot strengthening pages. More information for injuries and treatments foot pain and exercises.
BIBLIOGRAPHY
Wilson, J. J., & Furukawa, M. (2014). Evaluation of the Patient with Hip Pain. Am Fam Physician, 27-34.