
Tennis Elbow Treatments ( Lateral Epicondylitis) in Chandler AZ
Tennis Elbow Treatment in Chandler AZ
If you are a tennis, racquetball, or pickleball player, you may have experienced pain near your elbow joint, also known as "tennis elbow" or lateral epicondylitis. The term, "lateral," is confusing to those who are not familiar with medical anatomy. Although you may feel this pain towards the inside of your elbow, the term refers to the arm in the "anatomical position," in which the forearms are pronated, with the palms facing forward (see photo). The epicondyle is a bony protrusion at the end of the forearm bone, called the ulna. The extensor tendons involved in tennis elbow insert into the lateral epicondyle. While you may feel pain throughout your forearm, it is often most severe in this area.
What is Tennis Elbow?
Tennis elbow is an inflammation of the common extensor tendon, which is the attachment of several muscles that extend the wrist and fingers. Tennis elbow is typically an overuse (chronic) condition, as opposed to an acute injury. Many types of repetitive activities overwhelm the integrity of the tendon leading to damage and tendonosis.
Because it is a condition caused by poor body mechanics and overuse, tennis elbow rarely goes away on its own. Untreated, it can last up to two years, even if you rest the area. The good news is that treatment doesn't necessarily involve surgery. Physical therapy including extracorporeal shock wave treatment, Graston Technique, corrective exercises and pain reduction techniques such as class IV cold laser, electric therapy, and frequent icing can bring the condition under control.
Video: Tennis Elbow Injury & Treatment
Symptoms of Tennis Elbow
Although a variety of injuries can cause forearm pain, the following symptoms point to tennis elbow, and warrant a call to your physical therapist/chiropractor:
- Onset of pain is most severe when playing racquet sports, lifting heavy objects or when you feel pain on the outside of the elbow during the eccentric (extension) phase of biceps curls.
- The pain may affect most of the forearm, but it is sharpest near the elbow, and typically affects only one arm.
- Pain is chronic; it does not completely subside with rest over a 48-hour period, or the pain subsides but immediately returns when you resume activities.
- The pain has lasted for at least a week.
- The pain interferes with your normal daily activities and recreational activities.
- You may occasionally see swelling or bruising on the outside of your elbow.

Who is at Risk for Tennis Elbow?
Tennis elbow is most prevalent among adults over 40 years of age, and seems to affect men and women equally. Although it affects primarily active individuals, it can also affect those who are less active, but who overuse their extensor muscles doing daily activities such as housework. Reasons for developing tennis elbow can include:
- A sudden increase in recreational activity (especially racquet sports or weightlifting).
- Engaging in an unfamiliar recreational activity with insufficient rest/recovery between sessions.
- Poor form serving and returning balls, or during the eccentric (extension) phase of biceps curls.
- Inadequate hydration, including electrolyte imbalances in extremely hot weather.
- Muscle imbalances in the forearm.
Available in the office or Amazon.
Home Treatments for Tennis Elbow
The best home treatment for tennis elbow is RICE: rest, ice, compression and elevation. Since this injury is caused by inflammation, it's important to get the swelling down. You cannot ice too often. We like the large gel ice packs because they can be molded around the elbow and they are reusable.
Your primary care physician may also recommend anti-inflammatory medications, such as NSAIDS (e.g. aspirin, Advil and Aleve), or acetaminophen (Tylenol).
Even though we love for people to be active (and encourage it), you will need to stop doing the activity that caused the problem, at least until therapy gets the condition under control. Think about this as a time to work on other types of fitness, such as strength and flexibility.
A compression sleeve can provide some support and also help to decrease the pain during your daily activities. Kinesio tape (also called KT tape) can also provide support in the area.
Active Treatments
Physical therapy, which includes massage, extracorporeal shock wave therapy and strengthening exercises can help to correct the muscle imbalances that caused the injury and reduce inflammation. Shock wave therapy breaks up adhesions along the tendon and muscles, so that they can heal more effectively.
Study Review for Tennis Elbow - Steroid, PRP, Shockwave therapy
Alternative Treatments
Exercises that strengthen both the forearm flexor and extensor muscles, upper arm muscles, shoulder and core can all help to resolve this injury. It is not unusual for athletes to develop muscle imbalances by playing a sport. For example, tennis elbow can result from a lack of shoulder strength, an imbalance between the flexor and extensor muscles in the forearm, and a lack of core strength that forces the person to overuse the forearm muscles.

Graston Technique in Chandler
Graston technique uses stainless steel instruments applied forcefully to the injured area to break up scar tissue. Essentially, the idea is to "re-injure" the area to recruit myoblasts and promote proper healing. The provider slides the Graston tool along the skin in the direction of the tendon and muscle to break up scar tissue by pulling the layers of tissue apart. The technique not only speeds up healing, but also quickly reduces pain.
Video: Graston Technique For Scar Tissue Pain
Shockwave Therapy
Shockwave therapy causes a very fast compression on the tissue, which effectively "stomps on the tissue." The sudden impact stretches the less flexible scar tissue and breaks it, triggering proper tissue repair. It produces a peak pressure over 1,000 times that of ultrasound waves to stimulate tissue repair and break up scar tissue. It is a very different treatment than ultrasound.
The treatment is not painful - much more comfortable than other treatments such as Graston Technique, ASTYM, or IASTM. These treatments also trigger tendon repair by activating the body's same tissue repair systems. Except Graston Technique and ASTYM utilize shearing and pulling across the scar tissue to tear it, which can cause bruising and excessive inflammation.
Video: Shockwave Therapy For Injuries
Class IV Cold Laser Therapy in Chandler
Cold laser is a light therapy that uses a laser beam to speed up the delivery of ATP (adenosine triphosphate- basically 'fuel' for your muscles) to the injured area. It is a non-invasive and painless treatment that significantly reduces recovery time for chronic musculoskeletal injuries.
A treatment session lasts about five minutes. Typically multiple treatments are required in order to effectively promote healing in the injured area.

What Is Tendinopathy
Tendinopathy is pain and reduced function of tendons. Often the injury is due to the culmination of multiple pathological processes rather than a single event. The chronic repetitive stress leads to loss of tissue integrity and subsequent tearing or rupture.
I like to compare chronic repetitive injuries as adding pennies to a penny jar. Some days you add 15 pennies, some days you take out five pennies. Over time there is a tendency to add more pennies than you are removing, and eventually the jar starts to overflow. The overflowing penny jar is your chronic repetitive stress injury. There was not a single event or day that filled the jar; instead, the jar became full after an accumulation of days and pennies.

Often people are adding pennies to their jar because of muscle weakness, fatigue, or injury in other parts of their body. In addition to removing existing pennies from the jar, treatment will focus on reducing the amount of pennies you are adding every day.
The amount of repetitive stress placed upon your body can be dramatically reduced by changing postures and habits. For example, a person with low back pain may be uncomfortable sitting, which causes him to slouch at the computer. The slouching was contributing to neck pain and headaches. Improving the lower back pain will allow a person to sit with better posture and thus strain the neck less during the day.
Damage To Tendons
Mechanical and physical stress on tendons pull on the fibers. Too much pulling causes tears in the fibers, or even "fraying." Tendons will try and heal and repair, but cannot always completely finish repairing before the next trauma or physical stress.
Most Achilles tendon ruptures occur when participating in sporting activities. Often the ruptures are low grade damage has occurred. Biopsies have shown chronic degenerative changes in most ruptured Achilles tendons. These cases could be classified as acute trauma of chronically degenerated tendons.
In simple terms, the Achilles tendon has been chronically irritated with repetitive activity that has not completely healed, and then the Achilles ruptures during activity with a specific incident.

Repetitive loading and activity can be detrimental to tendon structures. The tendon repair mechanisms do not have enough time to heal before the onset of the next microtrauma or physical stress. This leads to a compromised tendon that is more susceptive to rupture.
Internal or intrinsic factors can make an individual more or less likely to suffer from a tendon injury. Factors include age, sex, and disease, such as diabetes, rheumatoid arthritis, ore genetic predisposition. Your overall health and condition can alter tendon structures or your ability to heal.
Muscle And Tendon Structure
The anatomical structure of muscles is like a licorice pull-and-peel. One fiber is wrapped in a group of fibers called a fascicle. Each fascicle is wrapped in a group of fascicles to form a muscle bundle. All the fibers are wrapped in coverings called fascia.
The coverings wrap around the individual fiber and the entire bundle. Each of the fascial coverings are a potential source of scar tissue formation, which will limit how the fiber slides and moves. This also changes the stress and strain that the muscle can handle.

This is the tendon, which is completely made of fascia and does not have any contractile properties like muscle. The muscles and fibers eventually end in a tendon that attaches to the bone. The muscle fascial coverings become thickened and dense before they attach to the bone.
Muscle contraction causes joint movement by pulling one bone closer to the other. Tendons transmit the forces produced by the muscles to the bone. The tendon is like a big thick rope; the tendon fibers are all aligned in the same direction to absorb the pulling forces.
Tendon fibers are made of type I collagen. This is a thick fiber designed to absorb and transmit forces. Excessive stress and strain in the fibers cause damage. Microtears in tendons are like nicking the fibers with a razor blade which cuts the fiber or causes it to fray. The body will try and repair this damage with proper type I collagen or it will form a temporary scar tissue patch with type III collagen.
In addition to chronic repetitive stress, microtears can be caused by uneven force production that results in uneven tendon loading. The amount of force absorbed by the tendon and the uneven distribution of forces lead to micro trauma and repair.
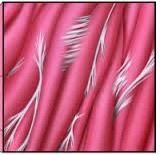
What are Scar Tissue And Fascial Adhesions?
Scar tissue forms when tissue does not heal correctly, or is under chronic repetitive stress. Scar tissue is weaker than normal muscle and connective tissue, which is why it becomes chronically sore with activity.
Scar tissue is like the body's duct tape; it is meant as a short term patch to help support tissue. However, in some cases the scar tissue is not replaced with normal type I collagen fibers. Instead, a weaker type III collagen is used as the duct tape.
Fascial adhesions are another term for scar tissue. Adhesions cause restrictions between the body's fascia. Stiffness, loss of normal range of motion and chronic pain develops from the type III collagen patches of fascial adhesions.
The next time a scar tissue patch undergoes stress and strain, it becomes aggravated and flares up. This process causes more scar tissue to be added to the outside of the patch and the process repeats itself over and over, leading to larger accumulation of scar tissue patches.
I like to describe these larger scar tissue patches as "onions." Scar tissue ends up growing in layers around the initial injury. Stress to the area aggravates the outside layers and triggers another layer to be formed. The layers further from the center are easier to aggravate than the inside layers, which is why the onion continues to grow in size without causing the inside area to properly repair.
Think of a chronic injury or area that bothers you. The same weak spot always flares up, whether it is in your low back, neck, or knee. The pain always seems to start in the same place over the years. This source of continued pain is a "scar tissue onion" or weak spot that keeps flaring up.
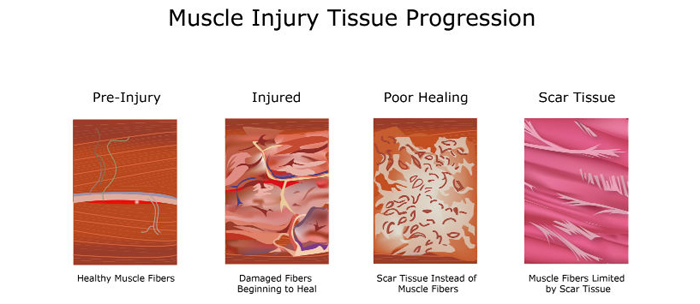
Causes of Scar Tissue
Four Common Causes of Scar Tissue
- Trauma - Sudden accident. Injuries like stepping off a curb or falling off a ladder.
- Repetitive Motion Injury - Same motion over and over.
- Improper Mechanics - Slouching at a computer makes muscles work harder to hold up your head, neck, and shoulders.
- Aging - Years of wear and tear on the body adds up.
In the end, any scar tissue that limits movement and causes pain needs to be broken up to restore normal motion.
That was the simple version.
A more complex and histological description of tendinopathy would include decreased oxygen and blood flow to the injured area. Tissue oxidative stress further decreases tissue repair and increases inflammatory cytokines. Tenocytes can produce substance P, catecholamines, glutamate, and acetylcholine.
Additional tissue repair cells play a role in tendon repair. Tenocytes within the tendon and sheath activate healing. Neutrophils and macrophages play a role in removing tissue debris and release chemicals that lead to the next phase of tissue repair.
The weaker scar tissue patch is made of type III collagen. In an ideal situation, the next repair phase transitions the type III to type I collagen, and this can continue for years beyond the original injury.

Is One Therapy Better Than Another For Chronic Tendinopathy?
No single therapy is consistently more effective than others. Sorry!
Multiple therapies are often required for chronic tendinopathy repair and healing. We utilize shockwave therapy, Graston Technique, and class IV low level laser therapy to enhance tissue repair. Proper treatment and rehabilitation of tendinopathy injuries often requires incorporating exercises and stretches to increase muscle flexibility and strength. Then teaching the body how to use those muscles again properly. Muscle pattern and joint stability exercises can help prevent future injuries.
Exercises & Stretching
Exercises are very important to rebuilding tendons and muscles, and encouraging proper collagen fiber alignment. The trick is performing the correct exercises at the right time. Most people overshoot with the exercises, performing too many repetitions, sets, or mechanical loading. Start slow and progress after mastering the easy exercise.
Medical and Alternative Treatments
For recalcitrant pain, your primary care provider may recommend a corticosteroid injection in the area. The injection instantly reduces pain and inflammation, and may enable you to more aggressively pursue physical therapy and rehabilitative exercises.
There is also evidence for the efficacy of acupuncture treatments in treating tennis elbow.